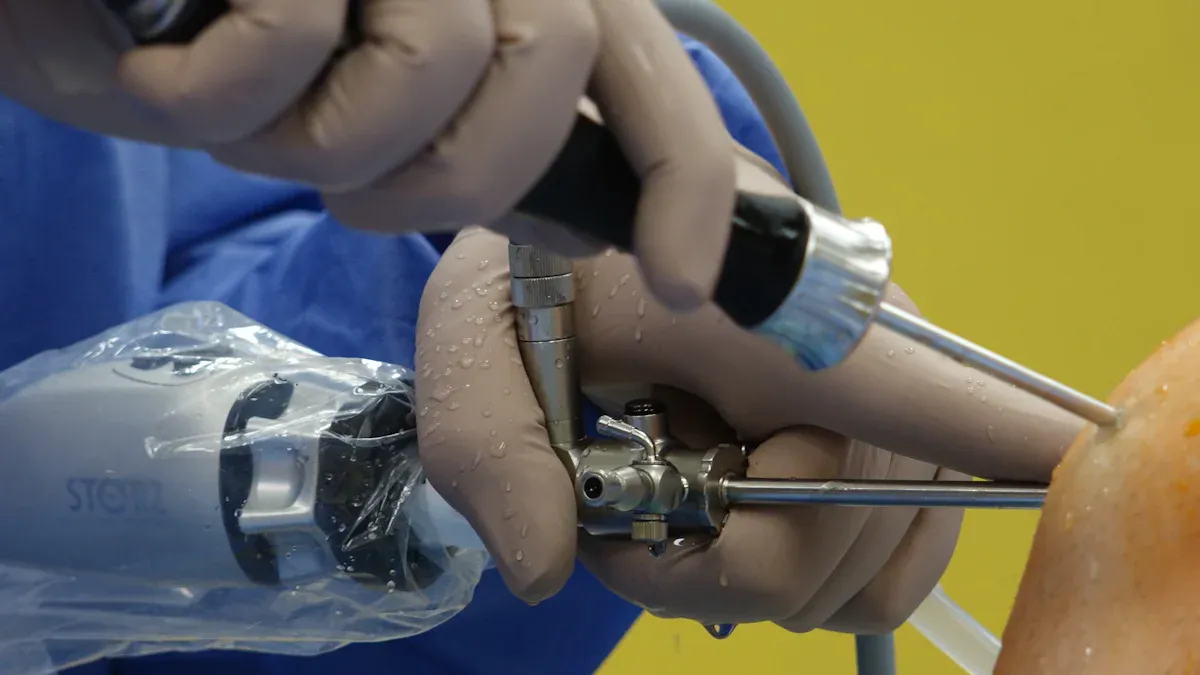
An endoscope serves as a specialized medical device that allows physicians to visually examine internal organs and tissues without major surgery. This tool features a flexible design, enabling access to hard-to-reach areas and providing real-time visualization during diagnostic and therapeutic procedures.
- In 2025, the global endoscopes market is projected to reach USD 26.36 billion, with a compound annual growth rate of 4.88% through 2030.
- Over 45 million endoscopic procedures occur worldwide each year, driven by rising chronic diseases, an aging population, and advances in healthcare infrastructure.
Understanding these advancements helps patients and industry professionals make informed decisions in a rapidly evolving medical landscape.
Key Takeaways
- Endoscopes allow doctors to examine internal organs without major surgery, leading to less pain and quicker recovery for patients.
- The endoscope market is expected to grow significantly, reaching USD 26.36 billion by 2025, driven by advances in healthcare and rising chronic diseases.
- Modern endoscopes feature advanced imaging technologies, improving diagnostic accuracy and enabling minimally invasive procedures.
- Proper preparation and recovery protocols are essential for patient safety during endoscopic procedures, ensuring optimal outcomes.
- Innovations in endoscope design, including AI and robotics, enhance the effectiveness of procedures and improve patient care.
Endoscope basics
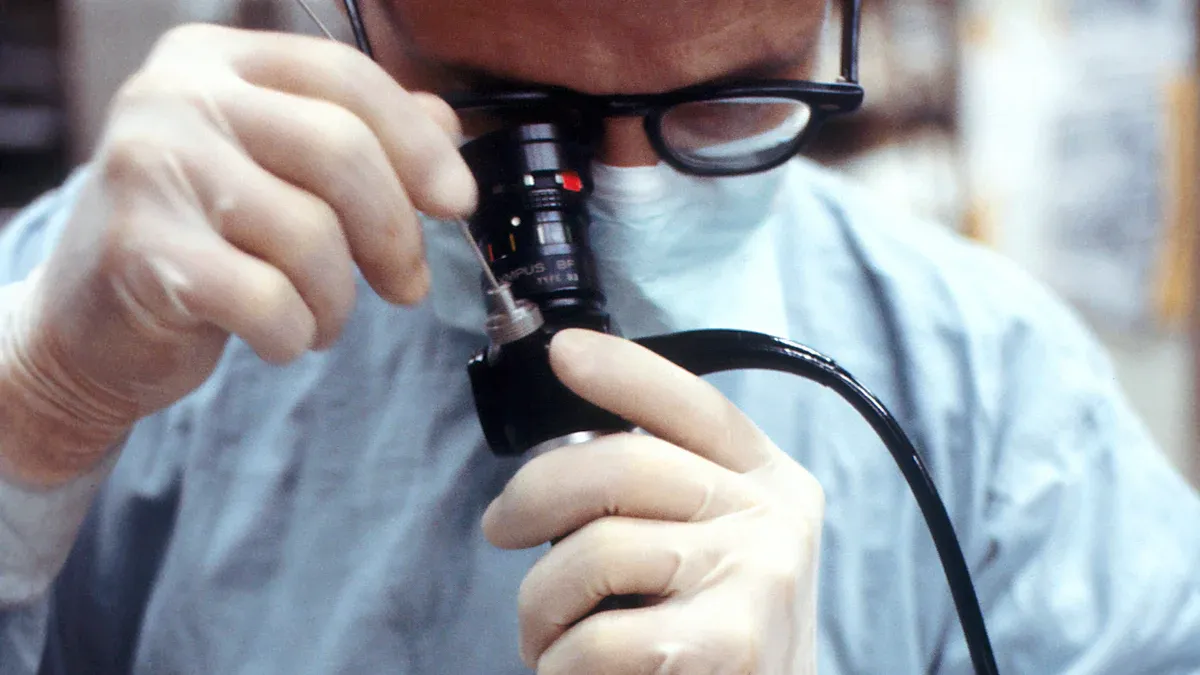
What is an endoscope
An endoscope represents a specialized medical instrument designed for internal visualization of organs and tissues. Medical professionals rely on this device to diagnose, monitor, and treat a wide range of conditions without the need for invasive surgery. The ISO 8600-1 standard defines the field of view of an endoscope as the vertex angle of the cone whose vertex is at the distal window surface, emphasizing the precision of its optical capabilities.
Note: The flexible design of an endoscope allows clinicians to access complex anatomical regions, improving diagnostic accuracy and patient comfort.
Key features of an endoscope include:
- Real-time imaging for immediate assessment.
- Flexible maneuverability for reaching difficult areas.
- Integration with advanced imaging technologies for enhanced visualization.
How endoscopes work
Modern endoscopes operate through a sophisticated combination of mechanical, optical, and electronic systems. The device consists of several primary components, each contributing to its functionality and effectiveness during medical procedures.
| Component | Description |
|---|---|
| Control Section | Contains knobs for controlling the camera, lights, and attachments, and maneuvers the device safely. |
| Insertion Tube | A flexible tube that enters the patient’s body, containing channels for water, suction, and imaging. |
| Optical System | Includes lenses and lights for capturing and transmitting images. |
| Camera and Imaging | Captures high-quality images and video footage for visualization and documentation. |
| Bending Section | Allows flexibility in navigating through the body. |
| Instrument Channels | Channels for passing instruments through the endoscope. |
| Water and Air | Channels for delivering water and air during procedures. |
| Suction Ports | Ports for suctioning fluids during the examination. |
A basic endoscope system typically includes the endoscope itself, a light source, an air pump, a video camera, and a video monitor. These components form an imaging chain that determines the quality of the displayed image.
The flexible design enhances maneuverability, enabling clinicians to reach intricate anatomical structures with minimal discomfort for the patient. Steerability features, such as control handles and 360-degree rotation, provide precision during procedures. The evolution of flexible endoscopes has transformed medical practices, especially in gastroenterology and surgery, by supporting minimally invasive techniques. These advancements result in less trauma, faster recovery, and reduced postoperative pain.
Endoscopes utilize advanced imaging technologies to deliver clear and detailed internal views. The following table outlines the main imaging technologies used:
| Technology Type | Description |
|---|---|
| Camera Sensors | High Definition (HD), FullHD, and Ultra HD (UHD) sensors, including CCD and CMOS technologies. |
| Light Sources | Colored LEDs, Xenon, and Halogen lights with filters. |
| Enhancement Technologies | Narrow Band Imaging (NBI), Autofluorescence (AF), and Flexible Spectral Imaging Color Enhancement (FICE). |
Medical professionals select the appropriate endoscope and imaging technology based on the clinical requirements and the area of examination. The continuous improvement in image quality and device design supports advanced procedures, such as natural orifice transluminal endoscopic surgery, which further reduces surgical trauma and improves patient outcomes.
Uses and types
Medical uses
Doctors use endoscopes to diagnose and treat a wide range of medical conditions. These devices help specialists visualize internal organs, collect tissue samples, and perform minimally invasive procedures. Patients benefit from less pain, shorter recovery times, and fewer complications compared to traditional surgery.
Note: Endoscopic procedures often result in smaller incisions, reduced blood loss, and faster healing.
Common conditions diagnosed or treated with endoscopic techniques include:
- Gastroesophageal Reflux Disease (GERD)
- Peptic Ulcers
- Barrett’s Esophagus
- Celiac Disease
- Inflammatory Bowel Disease (IBD)
- Colorectal Polyps and Cancer
- Esophageal and Gastric Cancers
- Gallbladder and Biliary Diseases
- Pancreatitis
- Helicobacter Pylori Infection
- Swallowing Disorders (Dysphagia)
Doctors often compare endoscopic procedures to traditional surgical methods. The table below highlights key differences in patient outcomes:
| Outcome | Endoscopic Group | Traditional Group | Significance |
|---|---|---|---|
| Operative Time | Longer | Shorter | P < 0.05 |
| Intra-operative Blood Loss | Lower | Higher | P < 0.05 |
| Duration of Drainage | Shorter | Longer | P < 0.05 |
| Length of Incision | Shorter | Longer | P < 0.05 |
| Short-term Complications | Fewer | More | P < 0.05 |
| Long-term Outcomes | Comparable | Comparable | P > 0.05 |
Main types of endoscopes
Endoscopes come in several main categories, each designed for specific clinical or industrial applications. The table below summarizes the primary types used in practice:
| Main Categories of Endoscopes | Description |
|---|---|
| Industrial Endoscopes | Used in industrial applications |
| Medical Endoscopes | Used in clinical practice |
| Rigid Tube Endoscopes | Rigid structure for precision |
| Optical Fiber Endoscopes | Tube type using optical fibers |
| Electronic Endoscopes | Utilize electronic imaging technology |
| Rigid Mirrors | Common in the market |
| Flexible Mirrors | Widely used in clinical settings |
Medical professionals select between rigid and flexible endoscopes based on the procedure. Rigid endoscopes provide stable, clear images and suit high-precision surgeries. Flexible endoscopes bend with the body, allowing access to complex anatomical regions. This versatility supports a broad range of diagnostic and therapeutic interventions.
Endoscopic procedures
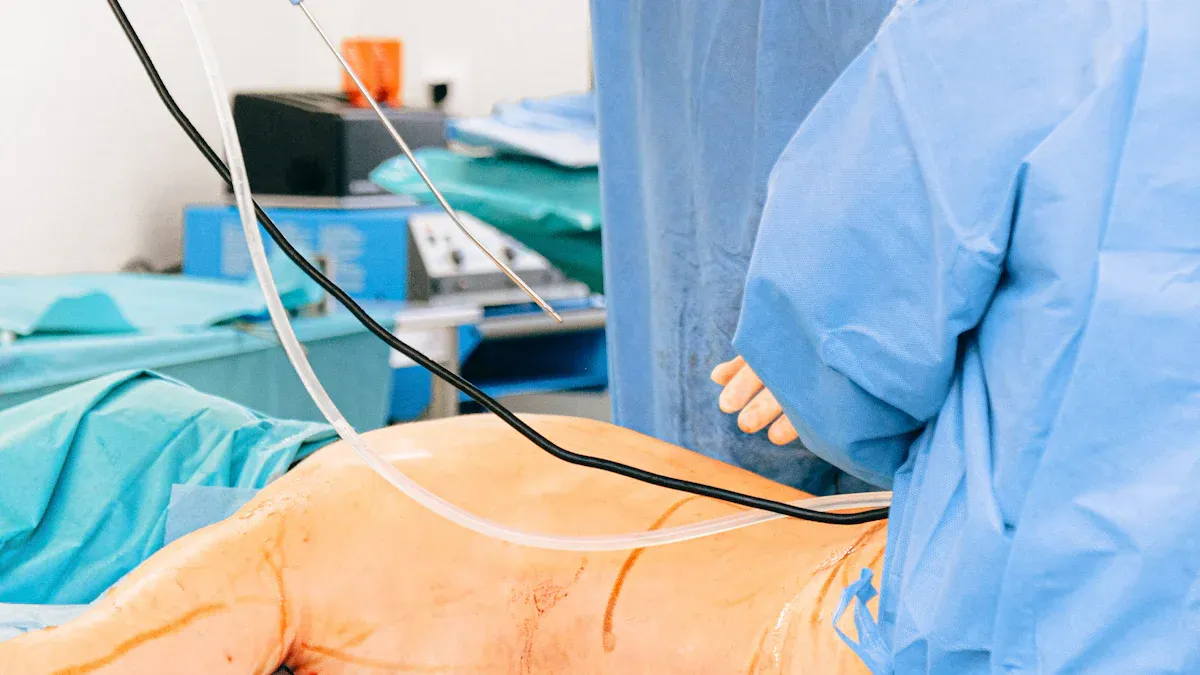
Preparation
Proper preparation ensures patient safety and optimal outcomes during endoscopic procedures. Medical teams follow a structured protocol before the procedure begins:
- Confirm patient identity, procedure type, and indication.
- Obtain informed consent.
- Conduct a thorough history and physical examination.
- Assess risk and plan sedation.
- Administer antibiotic prophylaxis if indicated.
- Review anticoagulant and antiplatelet medications.
- Set up patient monitoring devices.
- Prepare for emergency situations.
- Perform a final time-out to verify all details.
Tip: Patients should follow specific fasting instructions and disclose all medications to their healthcare provider.
What happens during
During the procedure, clinicians use an endoscope to visualize internal organs. The process typically follows these steps:
- The physician guides the endoscope through the mouth into the esophagus, stomach, and duodenum.
- Air is gently pumped to expand the area for better visibility.
- Real-time images appear on a video monitor, allowing the team to identify abnormalities or perform treatments.
- The physician may remove small tissue samples for biopsy.
- Treatments, such as removing polyps or stopping bleeding, may occur as needed.
Most procedures last 5 to 15 minutes. However, the total time at the facility, including preparation and recovery, averages about two hours. Factors such as the complexity of the anatomy or the need for immediate intervention can influence the duration.
Note: Common risks include sore throat, sedation effects, bleeding, perforation, and rare infectious complications.
Recovery
Recovery after endoscopy is usually brief. Patients spend at least 30 minutes in the recovery area under observation. Family members may join during this time. Before discharge, staff provide post-procedure instructions and contact information for follow-up. The table below outlines average recovery times for common procedures:
| Procedure Type | Average Recovery Time |
|---|---|
| Endoscopic Discectomy | 1-2 weeks for non-active jobs; 4-6 weeks for active jobs |
| Endoscopic Rhizotomy | A few weeks, with most patients returning to work in a few days |
| Open Spinal Surgery | Up to 12 months recovery |
| Endoscopic Foraminoplasty | Back to work in a few days |
Most patients resume normal activities quickly, especially after minimally invasive procedures.
Endoscope advancements in 2025
New technologies
The year 2025 marks a significant leap in endoscopic technology. Medical device manufacturers have introduced advanced imaging systems and innovative features that enhance both diagnostic and therapeutic capabilities. The following table highlights some of the most notable advancements:
| Advancement Type | Description |
|---|---|
| ELUXEO 8000 Endoscopic Imaging System | Delivers superior image quality, expanded therapeutic options, and streamlined workflows. |
| Amber-red Color Imaging (ACI) | Improves visualization of blood vessels and active bleeding by emphasizing color differences. |
| EUS Technology | Advances in Endoscopic Ultrasound (EUS) provide greater diagnostic precision. |
| Double Balloon Enteroscopes | New designs increase procedural effectiveness and access to challenging anatomy. |
Engineers have also integrated ultra-thin, high-resolution endoscopes, which allow clinicians to reach deeper anatomical regions with improved visual clarity. Disposable endoscopes now play a crucial role in reducing cross-contamination risks, supporting infection control in healthcare settings. Lighter and more ergonomic designs help reduce surgeon fatigue during lengthy procedures.
Artificial intelligence (AI) and robotics have transformed endoscopic procedures. AI-powered image analysis enhances lesion detection and supports more accurate diagnoses. Robotic systems improve maneuverability, enabling precise control and better patient outcomes. Capsule endoscopy models now use AI for optical diagnosis of colonic lesions, optimizing sensitivity and efficiency. Robot-assisted navigation and devices like EndoMaster have demonstrated improved safety and performance in complex interventions.
Manufacturing innovations
Manufacturers have adopted new materials and processes to boost endoscope durability and performance. The integration of robust materials increases resilience, allowing devices to withstand repeated use and harsh conditions. High-definition (HD) and ultra-high-definition (UHD) cameras provide sharper images, supporting more accurate clinical decisions. AI and machine learning further improve defect detection and operational efficiency.
Innovations in manufacturing, such as wireless connectivity and advanced imaging, have raised the quality and efficiency of endoscopes. These improvements contribute to better diagnostic accuracy and support the growing demand for minimally invasive procedures. Although advanced technologies can increase costs, the expansion of healthcare infrastructure and the prevalence of chronic diseases have made endoscopic procedures more accessible worldwide.
Endowista stands out as a leader in this evolving landscape. The company offers a comprehensive range of flexible endoscopes and essential components, utilizing advanced techniques like CNC machining and femtosecond laser processing. Two dedicated R&D centers, staffed by over 40 engineers, focus on next-generation device development. Endowista collaborates with partners in more than 30 countries, providing tailored solutions and regulatory guidance. These partnerships help clients reduce costs, save time, and minimize risks.
Endowista’s global reach and one-stop lifecycle services empower medical innovators to launch products efficiently and meet international standards. These partnerships unlock smarter healthcare solutions and drive measurable improvements in patient care and operational performance.
Industry trends
The endoscope industry in 2025 demonstrates robust growth and dynamic trends. The U.S. market is projected to expand from USD 5.19 billion in 2025 to approximately USD 11.22 billion by 2034, reflecting a compound annual growth rate (CAGR) of 9.00%. Flexible endoscopes represent a key growth segment, with the market expected to rise from USD 2.31 billion in 2024 to USD 3.75 billion by 2034, driven by a CAGR of 4.97%.
Healthcare providers increasingly rely on endoscopic procedures in emergency and intensive care settings, where rapid and accurate diagnosis is critical. The flexible endoscopes segment is the fastest-growing, particularly in urgent medical situations.
Regulatory changes also shape the industry. Switzerland’s 2025 update on good practices for endoscope reprocessing clarifies legal duties and aligns hygiene standards with the latest science. The European Union’s 2025 guidance on the classification of medical devices introduces updates under MDR and IVDR, including new rules for electronic instructions for use. These changes reduce uncertainty for manufacturers and accelerate market access across the EU.
Quality improvements in endoscope components have enhanced patient safety and outcomes. Healthcare-associated outbreaks linked to contaminated endoscopes have prompted stricter safety measures. Proposals to include endoscope-associated infections as a reportable quality measure incentivize hospitals to improve safety protocols and reduce infection rates.
Understanding endoscopes and their rapid advancements in 2025 empowers both patients and industry professionals to make informed decisions. Patients benefit from less invasive procedures, faster recovery, and high satisfaction rates. The table below highlights key benefits and risks:
| Benefit/Risk | Description |
|---|---|
| Revisional Endoscopy | Enables effective treatment after failed bariatric surgery without invasive reoperation. |
| New Devices | Innovative platforms reduce complexity and patient risk. |
| Sustained Results | Endoscopic sleeve gastroplasty achieves durable weight loss with minimal complications. |
Industry professionals should evaluate image quality, compliance, compatibility, reliability, and total cost of ownership when selecting partners.
- Ask about certifications and references.
- Confirm training and support services.
Patients and professionals can access resources like ASGE guidelines for expert advice and up-to-date information on endoscopic procedures.
FAQ
What is the main advantage of flexible endoscopes?
Flexible endoscopes allow physicians to access complex anatomical regions with minimal discomfort. These devices support minimally invasive procedures, which help patients recover faster and experience fewer complications.
How does Endowista support regulatory compliance for endoscope manufacturing?
Endowista provides regulatory guidance throughout the product lifecycle. The team assists with product registration, documentation, and compliance with international standards, ensuring smooth market entry for medical device companies.
Are disposable endoscopes safe for clinical use?
Disposable endoscopes reduce the risk of cross-contamination. Hospitals use them to enhance infection control, especially in high-risk environments. These devices meet strict safety and quality standards.
What training does Endowista offer for endoscope assembly?
Endowista delivers comprehensive assembly training and after-sales support. The company empowers client teams with hands-on instruction, ensuring proper device handling and maintenance.

