Endoscopes serve as essential medical tools that allow doctors to view internal organs without making large incisions. These instruments help detect and treat various conditions with minimal discomfort. Patients and medical professionals benefit from understanding their role, as endoscopic procedures offer faster recovery and fewer complications compared to traditional surgery.
- Over 191 million endoscopic procedures are performed globally each year, with numbers rising as hospitals adopt advanced technology.
- Smaller incisions and reduced tissue damage lead to quicker recovery and lower risk for patients.
Key Takeaways
- Endoscopes allow doctors to see inside the body without large cuts, leading to less pain and faster recovery for patients.
- These tools help diagnose many conditions, such as ulcers and cancers, improving patient outcomes through early detection.
- Endoscopic procedures are safer than traditional surgeries, with lower risks of complications and shorter hospital stays.
- Patients should follow preparation steps before an endoscopy to ensure the procedure goes smoothly and effectively.
- After an endoscopy, it’s important to monitor for any unusual symptoms and follow the doctor’s aftercare instructions for a safe recovery.
Main Uses of Endoscopes
Diagnosis and Screening
Endoscopes play a vital role in diagnosing a wide range of medical conditions. Physicians use these instruments to visually examine internal organs and collect tissue samples for laboratory analysis. Many gastrointestinal disorders can be detected early through endoscopic procedures, which improves patient outcomes.
Some of the most common conditions diagnosed with endoscopes include:
- Gastroesophageal reflux disease (GERD)
- Peptic ulcers
- Stomach cancer
- Celiac disease
- Colorectal polyps
- Inflammatory bowel disease (IBD)
- Esophageal and gastric cancers
- Pancreatitis
- Helicobacter pylori infection
- Dysphagia
Routine colonoscopies help prevent colorectal cancer by identifying and removing polyps before they become malignant.
A recent study highlights the effectiveness of digestive endoscopy in early cancer detection:
| Study | Findings |
|---|---|
| Liang’s Research | Accuracy of digestive endoscopy in diagnosing early gastrointestinal cancer was 97.5%. |
| Gastrointestinal Endoscopy Study | Digestive endoscopy accurately identifies tumors, reduces misdiagnosis, and improves outcomes. |
Treatment and Surgery
Endoscopes are not limited to diagnosis. They also enable minimally invasive treatments and surgical procedures. Physicians can remove polyps, treat bleeding, and perform biopsies without large incisions. This approach reduces pain, shortens hospital stays, and speeds up recovery. Endoscopic surgery has become a preferred option for many patients because it lowers the risk of complications compared to traditional open surgery.
Monitoring Health
Long-term health monitoring is essential for patients with chronic conditions. Endoscopes provide high-definition imaging and allow for precise tissue sampling, which supports accurate diagnosis and treatment planning. Regular follow-up endoscopies help monitor ulcer healing, assess treatment responses, and detect early signs of disease recurrence. Timely interventions, such as endoscopic mucosal resection, can prevent disease progression and improve patient prognosis.
How Endoscopes Work
Key Components
Modern endoscopes rely on a combination of mechanical and optical parts to function effectively. Each component plays a specific role in ensuring accurate visualization and safe navigation within the body. The following table outlines the main mechanical components found in contemporary endoscopes:
| Component | Description |
|---|---|
| Insertion Tube | The flexible or rigid shaft that navigates through body passages to reach target areas. |
| Optical System | Includes lenses, mirrors, and light sources for capturing and transmitting images. |
| Camera and Imaging System | Captures high-quality images and video for real-time visualization and documentation. |
| Bending Section | Allows articulation and maneuverability within the body, consisting of interconnected segments. |
| Instrument Channels | Channels for introducing tools for diagnostic and therapeutic purposes. |
| Control Mechanisms | Mechanisms for manipulating the bending section and other functions of the endoscope. |
| Water and Air Channels | Channels for irrigation and insufflation to improve visualization during procedures. |
| Suction Port | Used for removing fluids or debris from the examined area. |
Engineers have improved the operation part for better angle adjustment and smoothness. They have also developed turning devices with linear actuators, which provide enhanced control. Some advanced systems now feature robot-assisted flexible endoscopy, simplifying operation and increasing precision. The insertion tube, made from durable materials, withstands repeated use. The bending section enables articulation, allowing the endoscope to navigate anatomical curves. Instrument channels support procedures such as biopsy sampling and fluid aspiration.
Imaging and Light Technology
Imaging and light technology form the core of endoscopic visualization. Coherent fiberoptic bundles transmit light efficiently in flexible endoscopes, delivering high-quality color images. Many devices use charge-coupled device (CCD) video chips at the distal tip, which enhance image capture and display. Flexible endoscopes often provide a wide field of view, typically greater than 70 degrees, which is crucial for navigating within the body and performing both diagnostic and surgical tasks.
Optical shape sensors, integrated into some endoscopes, offer real-time data on the instrument’s position and shape. This technology improves guidance during procedures and reduces complexity and duration, all without the need for radiation. LED light sources have become standard in modern endoscopes. These LEDs deliver exceptional clarity and brightness, which is essential for accurate diagnostics and procedures. The precise illumination from LEDs reduces the risk of errors, enhancing patient safety. LED cold light sources emit less heat than traditional halogen systems, which helps prevent thermal injury to internal tissues and extends operational life. Improved illumination quality further enhances procedural safety and image clarity.
Note: The integration of advanced imaging and lighting technologies ensures that clinicians can perform procedures with greater confidence and accuracy.
Flexible vs. Rigid Endoscopes
Clinicians select between flexible and rigid endoscopes based on the clinical application and anatomical requirements. Rigid endoscopes are primarily used for procedures such as microlaryngoscopy, providing high-quality imaging of areas like the vocal cords and subglottis. Flexible endoscopes offer greater accessibility, reaching various body parts including the ear, throat, urinary tract, lungs, intestines, and abdominal cavity.
Flexible endoscopy is less time-consuming and can often be performed under local anesthesia, making it suitable for adults. Rigid endoscopy may be preferable for children and is typically performed under general anesthesia. Both methods achieve high success rates for removing foreign bodies, with low complication rates.
Recent innovations have focused on increasing flexibility, maneuverability, and precision. Flexible designs and ergonomic controls enhance navigation through complex anatomy, reducing patient discomfort. Features such as variable stiffness and advanced torque control improve navigation precision. Ultra-thin, high-resolution endoscopes now provide access to hard-to-reach areas, improving visual clarity for diagnosis and treatment. Improved maneuverability leads to shorter procedure times and increased patient throughput. Lighter, more ergonomic designs help reduce surgeon fatigue during lengthy procedures.
Flexible endoscopes can bend and adjust angles, allowing for better navigation through natural body cavities. This agility enables clinicians to access areas that rigid endoscopes cannot reach, making flexible endoscopes a more sensitive diagnostic tool than many medical imaging techniques. The visual range of anatomical structures is significantly greater with flexible endoscopes, facilitating more effective diagnosis and treatment of gastrointestinal and pulmonary disorders.
Types of Endoscopes
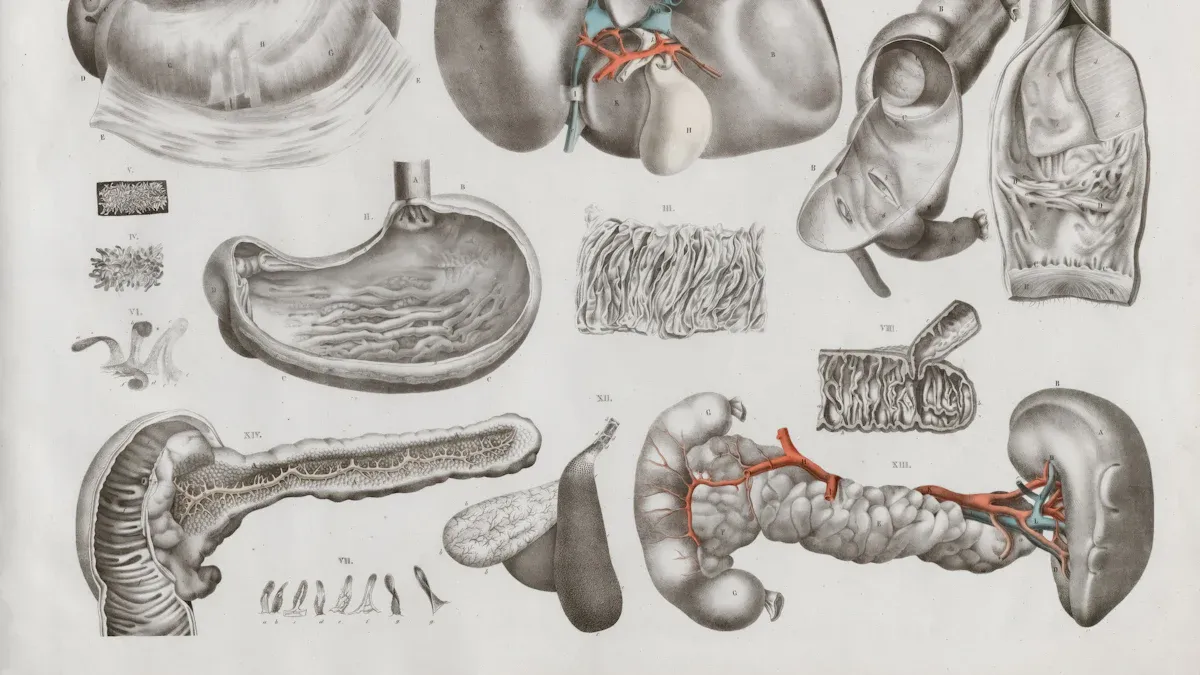
Gastrointestinal Endoscopes
Gastrointestinal endoscopes help physicians examine the digestive tract. These instruments include gastroscopes for the upper digestive tract and colonoscopes for the lower tract. Gastroscopes allow for the diagnosis of gastritis, ulcers, and reflux disease. Physicians use colonoscopes to screen for colorectal cancer and remove polyps. Upper endoscopy and colonoscopy rank among the most common procedures in hospitals.
Common gastrointestinal endoscopes include:
- Gastroscope
- Colonoscope
- Esophagoscope
- Sigmoidoscope
- Proctoscope
Routine use of these scopes enables early detection and treatment of digestive diseases, improving patient outcomes.
Bronchoscopes and Others
Bronchoscopes provide access to the airways and lungs. Pulmonologists use them to investigate chronic cough, biopsy lung tissue, and remove secretions or foreign bodies. Both flexible and rigid versions exist, each suited for specific clinical needs.
| Type of Scope | Main Uses | Key Features |
|---|---|---|
| Bronchoscope | – Investigates respiratory diseases – Biopsies lung tissue |
– Flexible and rigid options – Essential for lung care |
| Gastroscope | – Diagnoses upper GI disorders – Removes foreign bodies |
– Quick visualization – Used for therapeutic procedures |
Other commonly used endoscopes in clinical practice include:
- Laparoscope
- Arthroscope
- Cystoscope
- Laryngoscope
- Thoracoscope
These instruments expand the reach of minimally invasive medicine across multiple specialties.
Disposable and Specialized Endoscopes
Disposable endoscopes have gained popularity due to their sterility and convenience. They eliminate the risk of cross-contamination and reduce the need for complex cleaning. Hospitals often choose disposable models for high-infection-risk settings or emergency use.
| Aspect | Disposable Endoscopes | Reusable Endoscopes |
|---|---|---|
| Clinical Impact | Always sterile; portable and accessible | High image quality; advanced features for complex cases |
| Environmental Impact | Hard-to-recycle plastics; lower CO₂ per use | More resources for cleaning; lower annual CO₂ with frequent use |
| Financial Impact | No maintenance costs; no downtime | Higher initial and repair costs; more staff needed |
Specialized endoscopes address unique medical challenges. Advanced designs support complex therapies, such as tumor resections or bypassing blockages. Engineers have developed instruments with enhanced traction and grasping abilities, allowing for more effective interventions in difficult cases. These innovations help clinicians tailor procedures to the needs of specific patient populations.
Endoscopic Procedure: What to Expect
Preparation Steps
Proper preparation ensures a smooth and effective endoscopic procedure. Patients typically follow a series of steps in the days leading up to their appointment:
- Three days before: Patients should eat low-fiber foods and avoid high-fiber options.
- One day before: A clear liquid diet becomes necessary, and certain liquids must be avoided.
- Day of procedure: Patients bring identification and insurance cards and wear comfortable clothing.
- Medication management: Physicians provide instructions regarding blood thinners and other medications.
- Transportation: Arranging for a responsible adult to assist and provide transportation is essential.
Adhering to these guidelines improves the accuracy of the procedure and reduces the risk of complications. Studies show that patients who follow preparation instructions experience better outcomes and more appropriate follow-up care.
During the Procedure
Patients often experience a range of sensations during endoscopy. Many report feelings of trust in their medical team, which can foster a sense of control. Discomfort may occur, with pain levels varying from mild to severe. Sedation plays a key role in patient comfort. Nursing staff monitor patients closely, adjusting sedation as needed to ensure safety and minimize distress.
- Some patients sleep through the procedure due to effective sedation.
- Others may feel drowsy or groggy.
- Respectful communication from the medical team enhances the overall experience.
A well-trained team and proper sedation increase the likelihood of a successful and comfortable procedure.
Recovery and Aftercare
Recovery times differ based on the type of endoscopy performed. Most patients recover from anesthesia within 20–30 minutes. Mild sore throat or bloating may occur but usually resolves quickly. Patients should avoid driving, alcohol, and strenuous activity for at least 24 hours.
| Recommendation | Description |
|---|---|
| Monitor for complications | Watch for severe pain, fever, or swallowing issues. |
| Rest and hydration | Drink fluids and rest with head elevated. |
| Dietary adjustments | Start with clear liquids, then soft, bland foods. |
| Follow-up | Attend scheduled appointments for ongoing care. |
Promptly reporting new or worsening symptoms to a physician helps prevent complications and ensures a safe recovery.
Risks and Safety of Endoscopes
Common Risks
Endoscopic procedures offer many benefits, but they also carry some risks. Most patients experience only mild side effects, such as a sore throat or minor discomfort. However, more serious complications can occur. The most frequently reported risks include:
- Patient identification errors
- Pathology exam or report mistakes
- Gastrointestinal perforations or lacerations
- Bleeding
- Skin lesions
- Falls during recovery
- Medication errors
Doctors also monitor for rare but serious events, such as cardiopulmonary complications, missed lesions, and dental trauma. Gastrointestinal perforation and bleeding account for about half of all adverse events, while skin injuries and falls make up a smaller percentage.
| Complication Type | Endoscopic Surgery | Open Surgery |
|---|---|---|
| Surgical Complications | 0.5% | 7.9% |
| Neurologic Issues | 0.5% | 7.0% |
| Average Hospital Stay | 1.6 days | 3.7 days |
| Average Cost ($) | 66,815.90 | 146,271.21 |
Endoscopic procedures have a much lower complication rate than open surgery, making them a safer choice for many patients.
Minimizing Complications
Healthcare teams follow strict protocols to reduce the risk of infection and injury during endoscopy. These measures include:
- Immediate cleaning and high-level disinfection of endoscopes after each use
- Sterilization of instruments that break the mucosal barrier
- Use of personal protective equipment (PPE) such as gloves, gowns, and eye protection
- Rigorous hand hygiene before and after patient contact
- Environmental cleaning to prevent cross-contamination
A documented infection prevention plan guides staff actions. Regular training and teamwork improvements, such as Crew Resource Management, help reduce errors and enhance patient safety. Studies show that these safety measures can lower adverse event rates from over 21% to less than 4%.
When to Seek Help
Patients should watch for warning signs after an endoscopic procedure. Immediate medical attention is necessary if any of the following symptoms occur:
- Persistent or severe chest pain
- Difficulty breathing or swallowing
- Fever over 100.4°F (38°C) or chills
- Significant or ongoing bleeding, especially in vomit or stool
- Black or bloody stool
- Severe nausea or vomiting, especially with blood
- Pain that lasts more than 48 hours
Doctors provide clear, written instructions for aftercare and symptom monitoring. Timely follow-up and careful observation help ensure a safe recovery.
Endoscopes have transformed modern medicine by enabling doctors to diagnose, treat, and monitor conditions with precision. Patients benefit from several advantages:
- Minimally invasive procedures lead to less pain and faster recovery.
- Direct visualization ensures accurate diagnosis and immediate treatment.
- Most procedures remain safe and cost-effective, supporting ongoing health monitoring.
Patient satisfaction rates remain high, especially when sedation is used. For personalized guidance, individuals should consult healthcare professionals. Those interested in endoscopic technology can explore reputable medical websites or academic journals for further information.
FAQ
What conditions can doctors diagnose with endoscopes?
Doctors use endoscopes to identify digestive disorders, respiratory diseases, and some cancers. They also detect ulcers, polyps, and inflammation. Endoscopy helps confirm diagnoses and guides treatment plans for many chronic and acute medical conditions.
How long does an endoscopic procedure usually take?
Most endoscopic procedures last between 15 and 60 minutes. The duration depends on the type of examination and the complexity of the case. Some therapeutic procedures may require additional time for intervention.
Are endoscopic procedures painful?
Most patients report mild discomfort. Sedation or anesthesia reduces pain and anxiety. Medical teams monitor patients closely to ensure comfort throughout the procedure.
What are the main benefits of flexible endoscopes?
| Benefit | Description |
|---|---|
| Accessibility | Reaches complex anatomical areas |
| Comfort | Minimizes patient discomfort |
| Precision | Provides high-quality imaging |
| Versatility | Supports diagnosis and treatment |
Flexible endoscopes improve safety and efficiency in clinical practice.

